|
Getting your Trinity Audio player ready...
|
Botox injections are big business for medical practices. Before you start offering this service, make sure that you know the risks and requirements.
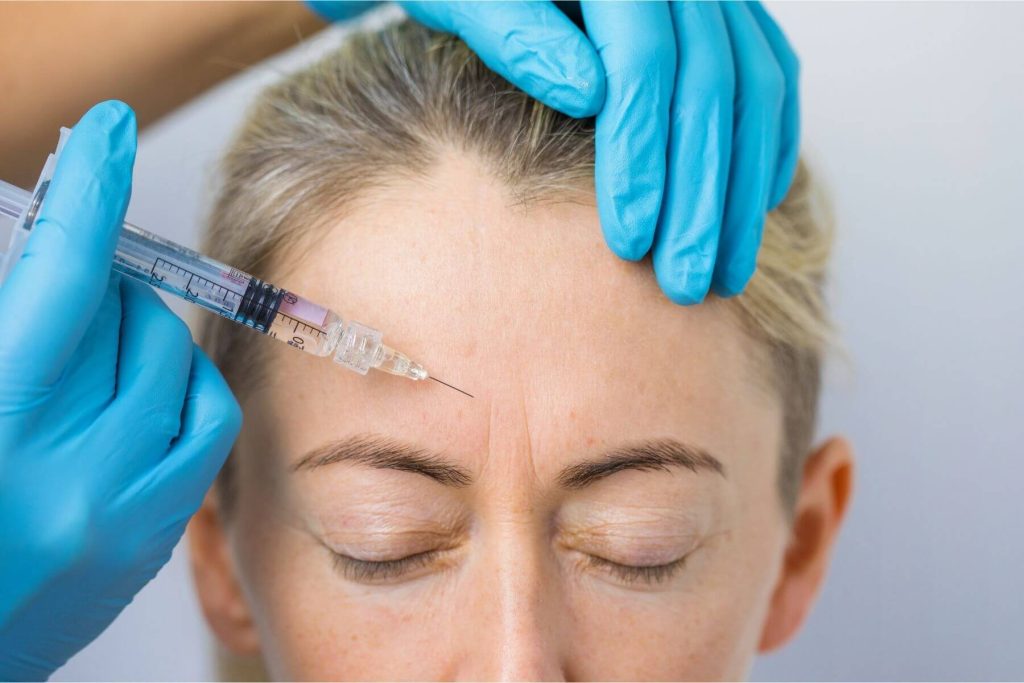
With the demand for Botox, Dysport, and other fillers increasing, many healthcare professionals view injectables as a promising revenue opportunity. The opportunity carries some risk, however. Learn about the most common sources of medical malpractice allegations or disciplinary actions that arise from performing Botox injections.
Injecting Botox: Four Key Ways to Land In Hot Water
A quick web search for “Botox malpractice” reveals that personal injury lawyers are eager to take on these cases. So let’s look at the most typical reasons for lawsuits and disciplinary actions.
Improperly Administered Botox
Providers — and many patients — know that improperly administered Botox can have grave consequences. While such complications are uncommon, the rise of non-physician injectors suggests that previous malpractice lawsuits may not be predictive of future cases.
It’s essential to be well-versed in the protocols set out by the drug manufacturer. Botox contains a toxin that can be harmful to the recipient. While off-label use is common, it must be carefully considered, demonstrative of evidence-based practices, and comprehensively documented in the patient’s record.
Insufficient Informed Consent Discussions
It’s also crucial that patients provide their informed consent to the procedure after a discussion about the potential side effects and medical complications. Clinicians should have these discussions repeatedly with patients receiving ongoing or routine injections. The Today Show detailed a woman’s experience with a drooping eye after a regularly-scheduled Botox treatment. Quoting the patient, the story reveals:
She noticed her left eye drooping. Panicked, [she] contacted the medical spa where she had the procedure done. “I spoke with the head plastic surgeon there and since he doesn’t specialize in injections, he referred me to someone else,” she explained.
This explanation casts doubt on the injectors’ supervision and training. The head physician was unable to counsel a patient with an adverse reaction. Thus, the patient later obtained medical treatment elsewhere. It’s then that she learned she was suffering from a condition that can result from improperly placed injections or over-dosage of Botox.
Regulators suspended the license of a New Jersey physician when it came to light that he had used fillers off-label for penile and breast enhancements. These procedures subsequently resulted in medical complications and even emergency surgeries for his patients. His records were inadequate, and his informed consent process was minimal to non-existent.
Inadequately Supervised Injectors
The relative safety and ease of Botox administration make it particularly susceptible to allegations of inadequate injector supervision. This situation places physicians and injectors at risk (and not just in the U.S.!).
Consequences for Physicians
For example, in 2021, the Illinois Department of Financial and Professional Regulation fined and disciplined a dermatologist whose non-physician employees injected patients when he wasn’t present. This disciplinary action shows why physicians should conduct initial patient consultations and supervise mid-levels or staff as required by law.
The supervision requirement varies by state. If the injections serve a medical purpose, the requirements may also vary by insurer. In Illinois, for example, various licensed medical professionals with proper training may perform Botox injections when supervised by a physician. But in California, only a physician, physician’s assistant, or registered nurse under the supervision of a physician may inject Botox.
Physicians who allow improperly licensed or supervised injectors to treat patients with Botox may also risk serious criminal charges for aiding and abetting the unlicensed practice of medicine. For instance, Multiple news stories document the case of a Florida physician who found himself in court after selling Botox to an unlicensed injector, who administered Botox in day spas and patient homes.
Consequences for Injectors
Improperly supervised injectors may face discipline for practicing medicine without a license — a criminalized offense in many states. For example, a recent Washington disciplinary report includes the following:
In November 2021, the Unlicensed Practice Program issued a notice of intent to issue a cease-and-desist order to [name omitted here] for unlicensed practice as a physician. [She] allegedly practiced medicine by injecting Botox into a person. [She] has no license allowing her to perform injections.
A news story from earlier last year revealed similar discipline taking place on the opposite coast. The Connecticut medical board reportedly disciplined a non-licensed individual who had been injecting Botox. And in Florida, a woman faced criminal charges (including 20 felonies) for posing as a nurse when administering Botox without a medical license.
Improperly Stored Medications
In a particularly egregious example, Rhode Island recently suspended a physician’s license after an investigation revealed that his practice stored Botox in a dangerous manner. In his practice refrigerator, investigators found an open box of Botox with a hypodermic needle sticking out of it. Such storage practices create grave infection and bacteria risks. The practice appears to have landed on investigators’ radar after they received a complaint detailing unsafely stored and expired medications.
A New Jersey physician also had his medical license suspended in late 2021 for multiple violations, including the storage of Botox in duffle bags. His practice had no medical-grade refrigerators on-site.
How Can You Make Sure Your Practice is Compliant?
Botox is a medical intervention using an FDA-regulated injectable medication. Thus, physicians and other injectors should approach these treatments with the requisite seriousness and professionalism. The cases highlighted here are merely illustrative of the complexities and risks inherent in patient care. Practices should do what they can to improve patient outcomes and minimize their risk.
- Consult with each patient to consider their complete medical history and obtain informed consent to the procedure.
- Follow the manufacturer’s instructions and maintain up-to-date education about the drug, appropriate dosing, and adverse outcomes.
- Ensure that all injectors act within their scope of practice and are properly supervised as required by state law.
- Implement standard operating procedures, or SOPs, to formalize the practice’s rigorous safety and compliance procedures.
If you’re a licensed healthcare professional looking to open a new medical spa or add cosmetic injections to your existing medical services, know the laws that govern this area. If you need guidance and operate in one of the states where we practice, book a consultation with one of our healthcare attorneys.
This blog is made for educational purposes and is not intended to be specific legal advice to any particular person. It does not create an attorney-client relationship between our firm and the reader and should not be used as a substitute for competent legal advice from a licensed attorney in your jurisdiction.